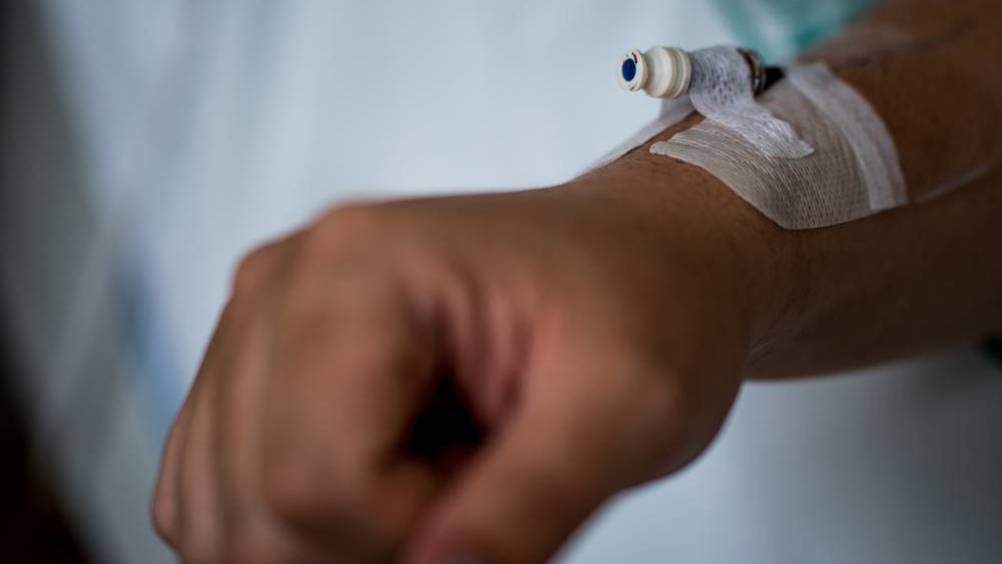
Emergency departments (EDs) have recently been experiencing an unprecedented surge in activity while our health economy resettles after the COVID-19 pandemic waves. This has led us to have to quickly rationalise and reframe how we provide our emergency care.
We know that peripheral IV cannulation (PIVC) is one of the most commonly performed invasive procedures in the ED. We also know that up to 40% of all PIVCs placed are not used or are used for only a secondary purpose, such as collection of blood samples (Thomas et al, 2020). IV access specialists have long advocated that IV access devices should only be placed if IV therapy is definitely required.
The first question of the Vessel Health Preservation Framework is whether there is a ‘genuine need for vascular access’ (Hallam, 2020). PIVC insertion can be painful for patients and comes with risks such as infection, bleeding and thrombosis. From an organisational perspective, it also adds cost and clinician time, both of which, in today's health economy, need to be carefully rationalised. So is it now time to actively challenge the notion of providing IV access ‘just in case’?
It seems hard to imagine that a patient would ever question why a clinician has placed a PIVC in them in an emergency situation, because a PIVC is often a precursor to life-saving treatment. But PIVCs are not a harmless intervention, so clinicians need to always carefully assess whether they are genuinely required. This can be difficult to do in a busy ED.
Interestingly, there appears to be very little evidence or guidance on who should receive a PIVC and when, while in the ED. This may be due to the vast and unpredictable cohort of patients who could present to an ED, which could potentially make this guidance large and difficult to navigate. Hawkins et al (2018) studied ED PIVC insertion and asked clinical staff to think critically and only place a PIVC if they believed there would be an 80% chance that it would be used in the next 24 hours. Clinicians were also asked to consider if the risk of the PIVC insertion outweighed the benefit. Using this approach resulted in a reduction of PIVC insertion by 9.8% and an increase in use of the PIVCs placed by 12.9%, which had a significant positive impact on cost and clinical time.
A review of the literature on ‘just-in case’ PIVC insertion in EDs (Gledstone-Brown and McHugh, 2018) concluded that the practice was associated with compromised patient safety, squandered finances and misdirected practitioner time. Cultures of convenience and shortfalls in PIVC-related education facilitated the prevalence of placed-then-unused PIVCs.
It seems that one of the main ways to improve this practice and reduce the number of unused PIVCs is through education and awareness programmes to promote best IV practice. Clinical staff need to be reminded that inserting a PIVC is not risk free and to be aware of the possible complications associated with inserting a PIVC, including beyond the ED. Staff need to consider alternative treatment methods.
Essentially, engaging with clinical staff to only place PIVCs if they are likely to be used would save clinical time, cost and an unnecessary invasive intervention on a patient, so it seems like a clear and easy win. However, if it was that easy it would already be being done. Reducing PIVC insertion in an ED would probably require a multimodal approach to reassure clinicians that the current practice of placing a PIVC ‘just in case’ is more time consuming than not, and is an unnecessary outdated practice. Achieving this may require a cultural shift in clinical thinking that would require whole department analysis and buy-in, which may be difficult to achieve. However, in 2021, we do need to critically evaluate all of our healthcare practices and challenge where our efficiencies are, and reducing ‘just in case’ PIVC insertion certainly seems to be an area where we could quickly see positive results for both patients and clinicians.